The map below highlights the malaria areas in SA in 2017.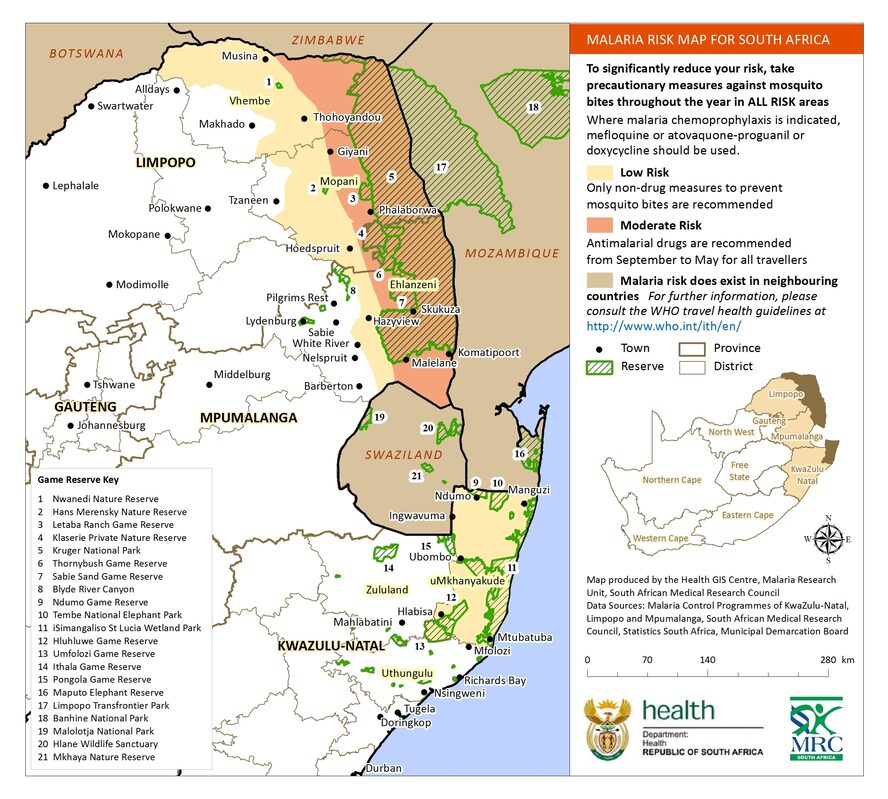
Malaria transmission occurs in three provinces in SA: KwaZulu Natal, Mpumalanga and Limpopo. Transmission is generally associated with higher rainfall and temperature, between September and May each year. Plasmodium falciparum infection accounts for about 90% of malaria diagnosed in South Africa.
The female Anopheles mosquitos which transmit malaria are only active and more likely to bite between dusk and dawn. Prevention of mosquito bites should be enforced between dusk and dawn.
Measures to prevent mosquito bites include:
- Wear long pants and socks
- Applying topical mosquito repellants to exposed skin areas that contain at least 20% DEET
- Burning of coils for repelling mosquitoe
- Sleeping under mosquito nets treated with long-lastinginsecticide when in high transmission area
- Use of air- conditioning and fans where available
- Staying in dwellings with screened windows and doors
Current recommended malaria prevention medication include mefloquine, doxycycline or atovaquone-proguanil. Your doctor will advise on the best option. Even though these medications are highly effective at preventing malaria, they are not 100% effective.
Anyone returning from a high risk malaria area ( up to one month) who has flu like symptoms must be screened for malaria.